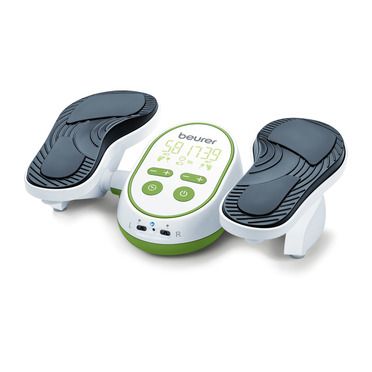
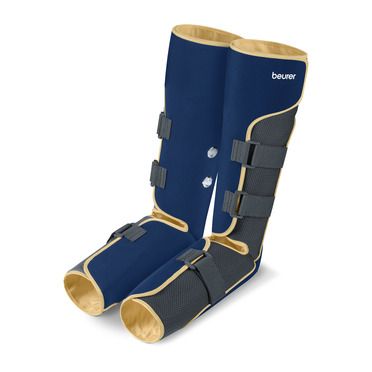
Verabschieden Sie sich von Rückenproblemen! Der Beurer Haltungstrainer PC 100 PostureControl wird einfach am Kleidungsstück angebracht und sendet ein sanftes Vibrationssignal bei zu langer eintöniger Sitzhaltung. So sitzen Sie aktiver und dynamischer und geben Rückenschmerzen keine Chance.
- Vorbeugung von Rückenproblemen
- Einfaches Anbringen am Kleidungsstück
- Von Physiotherapeuten und Medizinern empfohlen
- Feedback in Echtzeit
- Speicherkapazität: 14 Tage
- Bequeme und einfache Bedienung via „8sense“ App
- Mit Lithium-Ionen-Akku
| Produktbezeichnung | Haltungstrainer |
| Connect | ja |
| Leistung in Watt | 0,5 |
| Technologie | Vibrationssignal |
| CE | ja |
| Garantie (nähere Informationen in der Gebrauchsanleitung) | 2 |
| EAN | 4211125639501 |
| Artikelnummer | 63950 |
Ios
- iPhone 13 pro
- iPhone 13 pro max
- iPhone 13
- iPhone 13 mini
- iPhone 12 Pro Max
- iPhone 12 Pro
- iPhone 12
- iPhone 11
- iPhone Xs Max
- iPhone Xs
- iPhone XR
- iPhone X
- iPhone 8 Plus
- iPhone 8
- iPhone 7 Plus
- iPhone 7
- iPhone 6s Plus
- iPhone 6s
- iOS ≥ 14.0
Android
- Samsung Galaxy A32
- Samsung Galaxy A12
- Samsung Galaxy Z Flip3
- Samsung Galaxy S21
- Samsung Galaxy S20 FE
- Samsung Galaxy S9
- Google Pixel 4
- Huawei Mate 20
- Huawei P20 Pro
- Oppo reno4
- Poco X3 pro
- Android™ ≥ 8.0

Optimierte Sitzposition
Für eine bessere Rückengesundheit

Rückenproblemen vorbeugen
Der PC 100 hilft dabei Rückenprobleme vorzubeugen

Vibrationssignal
Sanftes Vibrationssignal bei zu langer eintöniger Sitzhaltung
8sense by Beurer
Geben Sie Rückenproblemen keine Chance!
Verabschieden Sie sich von Rückenproblemen! Der Beurer Haltungstrainer PC 100 PostureControl wird einfach am Kleidungsstück angebracht und sendet ein sanftes Vibrationssignal bei zu langer eintöniger Sitzhaltung. So sitzen Sie aktiver und dynamischer und geben Rückenschmerzen keine Chance.